What is genetic testing?
To understand genetic testing, lets start with a couple of buiding blocks.
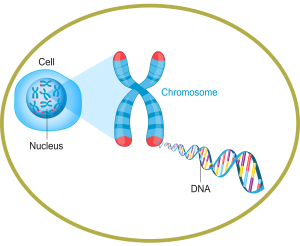
DNA (Deoxyribonucleic acid) is the hereditary material which we inherit from our parents. DNA functions like an instruction manual for the human body. It provides all of the instructions our bodies need for normal human growth and development. A gene is a specific instruction that tells the body how to make a specific protein. We have approximately 24,000 genes, meaning we are made from a complex mix of proteins that interact with each other and with the environment.
Genes are packaged into structures called chromosomes. Chromosomes are contained in cells, with most cells containing 23 pairs of chromosomes. Cells are the building blocks of living things. Our bodies are made up of a large number of cells and these perform many functions.
If the molecules making up a gene are altered, this can stop that gene from producing its regular protein because the “instruction” is no longer correct. This kind of alteration is called a mutation, or a pathogenic variant, and can result in an inherited genetic condition. For example, we have genes that produce proteins that control how quickly our cells replicate.
When these proteins are working they protect cells from becoming cancerous through controlling their growth. Individuals with a mutation in one of these ‘cancer protection genes’ may not have such effective cell growth control and have an increased risk for certain types of cancer. It is possible to inherit a mutation in a gene from a parent and so other family members may also have this increased chance of developing cancer.
Genetic testing
There are many forms of genetic testing.
- Ancestry testing
- Diet and fitness related testing
- Pharmacogenetic (drug) testing
- Cancer genetic testing
Cancer genetic testing
At the NZ Family Cancer Service, we provide a genetic testing service as part of a personalised cancer genetic risk assessment.
The information obtained from the family history assessment and testing can help to identify the best treatment options for those with cancer. Personalised risk assessment provides healthy people with the genetic information needed to make informed health care decisions appropriate for their level of risk. For example, women with BRCA1 or BRCA2 gene mutations have a high lifetime chance of developing breast and ovarian cancer and can choose preventative strategies.
Panel testing
Genetic testing capability continues to evolve as advances in testing are made. Until recently, testing of one or two genes at once was the norm. Now, laboratories offer multigene panels, which means many genes can be simultaneously tested.
BRCA genetic testing
Angelina Jolie is a well-known actress who had a major role in increasing the awareness of hereditary breast / ovarian cancer by sharing her own personal health journey. Angelina carries a BRCA1 mutation which increases her chance of developing breast and ovarian cancer. In 2013 she undertook a prophylactic double mastectomy and more recently a salpingo-oophorectomy (removal of fallopian tubes and ovaries).
Angelina chose this risk-management approach to significantly reduce her risk of developing breast and ovarian cancer. Such risk-reducing surgery is an option to consider by women who carry a BRCA mutation or have a strong family history of cancer.
Clinical utility
With the introduction of panels, we now have the ability to test multiple genes at the same time that may be associated with an inherited predisposition to cancer.
For some genes available on a panel, there may not be enough scientific evidence to understand the impact a mutation in one of these genes may have on an individual. This means that while a mutation may be detected, there is not sufficient information to help guide management choices.
At the New Zealand Family Cancer Service our ethos is to only recommend genes to be tested, where there is supporting medical management guidelines. Would you want to find out that you carry a mutation that might mean you have an increased risk of a particular cancer, and then find out that there is nothing that you can do to alter that risk?
A genetic counsellor can assess your family history of cancer and help guide gene selection, so that any decision to proceed with genetic testing makes sense based on your family history, and for your needs.
When your genetic test results are available, our genetic counsellors will interpret them for you, ensuring you understand any implications. They will also help you understand what follow-up is required, based on recommended guidelines.
Your privacy and informed consent
At NZ Family Cancer Service, we take privacy very seriously and at all times comply with the Health Information Privacy Code 1994 (2008 edition).
Our privacy policy can be read here.
We also take additional steps to ensure our partner laboratories also look after your personal information. We are all too aware of laboratories that provide testing services, and in the same breadth provide access to your information for commercial gain. At NZ Family Cancer Service our labs agree to strict criteria regarding the use of your personal information.
Informed consent
Prior to any testing, our genetic counsellors walk our patients through informed consent. This process gives people the information that enables them to make a decision about genetic testing. Further information about informed consent can be read here.
As part of our consent process we also disclose that we may share your anonymised information with 3rd parties for the purpose of scientific research, which may ultimately lead to improved care for patients. The more information that is available to researchers, the more it helps them better understand how different genetic mutations influence cancer.
The testing process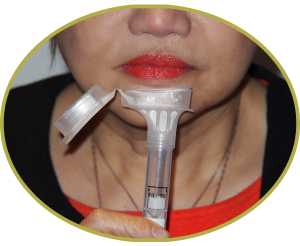
We made it easy for people to access genetic counsellors from the privacy of their own home, and we have done the same for genetic testing
Our testing process is simple and straightforward. We use a “saliva sample” as the mechanism for providing us with your DNA.
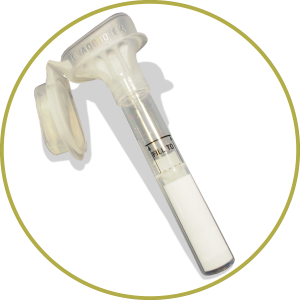
To facilitate this, we provide you with a genetic test kit supported by written and video-based instructions. Providing a saliva sample can be done from your own home, or where you are most comfortable. Once you have provided your sample, let us know and we will arrange for collection and dispatch to our laboratory.
The beauty of a saliva sample is its relative stability over a long period of time. Unlike blood, once your saliva sample is in the transport tube your it remains stable for a number of months at room temperature.
Results of your test
There are three possible results from the genetic testing:
- Positive test: The test identifies a gene mutation, confirming a hereditary susceptibility to specific types of cancer (the implications will depend on the gene involved). This information can be used to inform treatment and surveillance for you and for the wider family.
- Negative result: The test does not identify a gene mutation. This would be reassuring information and would indicate that a hereditary cancer syndrome is unlikely. We will provide screening advice for you and your family based on the test results and family history.
- Uncertain result: The test identifies an unclassified gene variant. This is a variation in which the clinical implications are not known at this time. Future research may help to clarify the meaning of this genetic variant. An uncertain result should be reviewed in the future. Until then we can provide advice on treatment and surveillance based on an individual’s symptoms, or family history of cancer.